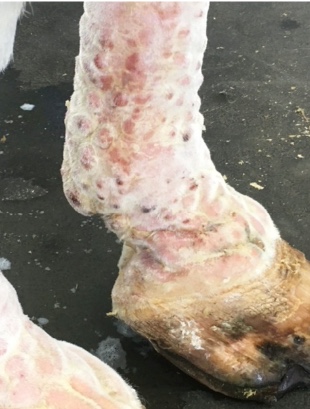
A swollen leg caused by cellulitis or lymphangitis is relatively common in the horse and can be very frustrating to treat. The two terms are often used interchangeably, and there is a close relation between these two conditions, and they are often concurrent. Once a horse has had cellulitis or lymphangitis, then recurrence is common, and the leg may remain swollen.
Many horses will “stock up” with fluid swelling (subcutaneous oedema) in two or more legs (usually hindlimbs). This is often a minor problem seen when horses are standing after a reduction in exercise or is sometimes associated with viral infections. Cellulitis and lymphangitis are dramatically different to “stocking up”– the horse presents with a hugely swollen leg (often a hindleg) and is often very lame. These conditions should be treated as an emergency rather than a wait-and-see approach as it can progress very quickly.
What is cellulitis and lymphangitis?
Cellulitis is inflammation of the deep dermis and subcutaneous tissues – the different layers within and under the skin.
Lymphangitis refers to inflammation of the lymphatic vessels. The lymphatic system drains fluid from the leg filtering through lymph nodes. In cases of lymphangitis, the lymphatic vessels and nodes become overwhelmed by infection.
In practice, these two terms are often used interchangeably and histologically; cellulitis often has evidence of lymphangitis. It can be quite difficult to differentiate between the two conditions; hence often, both terms may be used.
In some parts of the world, ulcerative lymphangitis occurs due to Corynebacterium pseudotuberculosis (worldwide) and Histoplasma farciminosum (Africa, Asia, Middle East).
For this article, given their closeness and similarities, lymphangitis will be considered as a form of cellulitis.
Primary and secondary cellulitis
What are the causes?
Cellulitis is caused by bacterial infections. In humans and horses, it is most commonly associated with staphylococcal or streptococcal bacteria – the most common one being Staphylococcus aureus.
Infection with Gram-positive bacteria is more common than infection with Gram-negative ones, but in some cases, mixed infections are present. Escherichia coli is sometimes found. The presence of E coli and mixed bacterial populations often contribute to a poorer prognosis. Some of the bacteria can contribute towards “toxic shock.” Occasionally fungal infections have been reported.
What are the symptoms?
Acute painful swelling
Both cellulitis and lymphangitis present as acute painful swelling in a single limb. Sometimes in lymphangitis cases, it is possible to visualise prominent superficial lymphatic vessels.
Heat and pain
There is heat and pain upon palpation with touch or pressure, causing a severe pain response.
Lameness
The lameness is often severe, with the horse reluctant to bear weight on the affected limb.
Discharge
Sometimes there is serum oozing from the leg.
Pyrexia
Horses may or may not have a high temperature.
High heart rate
A horse may or may not have a high heart rate from pain or a high temperature.
Ulcers/dead skin
The skin can become devitalised and slough, leaving gaping holes.
Complications
There are many other complications that can occur, including laminitis, osteomyelitis (bone infection), tissue necrosis, thrombosis, endotoxemia, septic arthritis, colitis, colic and extensive skin loss. The most common
How is cellulitis diagnosed?
Diagnosis is usually made on the basis of the clinical signs described earlier. Ultrasound and radiography are useful in confirming whether other structures are involved, such as tendons, ligaments and bones. Ultrasound can be used for detecting pockets of fluid that can be sampled for bacterial culture and antimicrobial sensitivity. Advanced imaging such as CT and MRI may be options in complicated and unresponsive cases but are not readily available here in all areas of Australia and are expensive. The bacterial culture and sensitivity tests are very helpful in confirming which bacteria are present and selecting the most appropriate antimicrobial – it is best performed BEFORE any antibiotics are administered, so don’t be tempted to administer any antibiotics that you may have around.
Antibiotics should only be administered to your horse under veterinary prescription.
Sometimes a blood culture may be performed – a blood sample is taken in a sterile fashion, and the blood is placed in a special growth media for culture.
Systemic blood samples may be taken to monitor white blood cell counts and inflammatory markers such as SAA and fibrinogen.
How is cellulitis treated?
Aggressive and early intervention is the key to a good outcome, so early veterinary attention is strongly advised.
Usually, a combination of antimicrobial therapy, anti-inflammatory drugs and analgesics are the main medications used.
Antimicrobials are often required for at least a week but sometimes for up to a couple of months. Different antimicrobials may be used according to the culture and sensitivity or response to treatment. These include penicillin, gentamicin, oxytetracycline, trimethoprim sulphadiazine combinations, doxycycline, rifampin, chloramphenicol and enrofloxacin. Antimicrobials should only be used under veterinary guidance and at appropriate doses – inappropriate use of antimicrobials is a key factor in the bacterial resistance issue in both human and veterinary medicine and is a very serious issue.
Nonsteroidal anti-inflammatory drugs (NSAIDs) are useful for both their pain relief action and their anti-inflammatory effect. The most common ones used are phenylbutazone or flunixin. On occasion, corticosteroids may be considered to reduce swelling and fibrosis, but the timing and use need to be very carefully selected.
Pain relief/analgesia is crucial, not only on welfare grounds but also to help prevent the development of contralateral limb laminitis. Other analgesics may be considered in combination with NSAIDs, particularly paracetamol. If the cases are hospitalised, then constant rate infusions of ketamine, opioids and lignocaine can be used, and epidural analgesia is another option.
Drainage of pockets may be considered if there is a large accumulation of fluids.
Icing or cold hosing may be considered but do not leave the leg wet.
Some cases may benefit from the use of daily pressure bandages, but these need to be carefully monitored so they do not contribute to pressure sores.
Light walking may be considered if the horse is not in too much pain, and qualified physiotherapists can sometimes help with exercises and lymphatic drainage massage, but this has to be very carefully applied and should not be performed without professional guidance.
What is the prognosis for cellulitis?
The prognosis is variable depending on the severity of the infection and other complications. The less severe cases have a good prognosis, but the serious ones can have a poor prognosis. Negative factors are pyrexia, skin wounds, mixed bacterial populations and laminitis.
Following recovery, horses may have structural damage within the soft tissues and may have persistent enlargement and change in contours of the leg to varying degrees; they also have an increased chance of recurrence.
FAQ
Is there a breed predisposition?
Cellulitis can occur in any breed, but a couple of studies have suggested that Thoroughbreds are overrepresented.
Is it more common in the fore or hindlimbs?
It seems that cellulitis is more common in the hindlimbs. It is assumed that this might be because hindlimbs are at a greater risk of trauma.
Summary
Cellulitis and lymphangitis are relatively common in the horse. They are bacterial infections within the skin, subcutaneous tissue and sometimes involve the lymphatic system. The main presentation is a large, swollen and painful leg with lameness, and it is often the hindlimbs that are involved. Treatment involves the use of NSAIDs and antimicrobials. Aggressive and early intervention is the key to a good outcome, so early veterinary attention is strongly advised; if you are suspicious your horse has cellulitis, don’t just wait – call your veterinarian as soon as possible.